![]()
[Image: Lasker Foundation]
The Lasker Foundation has bestowed its 2023 Lasker-DeBakey Clinical Research Award on James Fujimoto and Eric Swanson of the Massachusetts Institute of Technology (MIT) and David Huang of the Oregon Health & Science University, USA. The award cites their work in “the invention of optical coherence tomography, a technology that revolutionized ophthalmology—allowing rapid detection of diseases of the retina that impair vision.”
“America’s Nobels”
The Lasker Foundation awards—a series of distinctions awarded annually in basic medical research, clinical research, public service and “special achievement” in medicine—are among the world’s most significant recognitions in biomedical science. The awards were created and endowed by Mary Woodward Lasker and Albert David Lasker in 1945, with the specific aim of recognizing and celebrating biological and clinical advances that improve human health. The awards carry an honorarium of US$250,000.
The Lasker awards have been called “America’s Nobels,” and a large number of previous Lasker laureates have indeed later found themselves tapped as well by the Nobel Assembly. Recent examples include James Allison, the 2015 Lasker winner in the clinical category, who went on to share the 2018 Nobel Prize in Physiology or Medicine for his work in cancer immunotherapy; and William Kaelin, Peter J. Ratcliffe and Gregg Semenza, honored with the 2016 Laskin award in the basic-research category for their work on oxygen sensing by cells, which later also snagged the 2019 Nobel Prize.

James Fujimoto, David Huang and Eric Swanson. [Images: Jake Belcher, MIT / Oregon Health and Science University and Lasker Foundation / Lasker Foundation]
From interferometry to retinal imaging
The work by Fujimoto, Huang and Swanson honored in this year’s clinical award unfolded during the late 1980s and early 1990s in Fujimoto’s lab at MIT. It grew out of efforts to use low-coherence interferometry (LCI) to measure the time delay of optical pulses echoed from tissues at depth—analogous to ultrasound imaging. (At the time, parallel efforts were also afoot at the University of Vienna, Austria, to leverage LCI for ophthalmic problems such as measuring eye length.)
Fujimoto—an expert in ultrashort-pulse lasers, who cut his scientific teeth in the MIT lab of Erich Ippen—originally tried to put such lasers into service in the problem of seeing tissues at depth using “echoes of light.” But while these efforts were promising, they proved to be too slow and expensive to be practical (at least with the equipment of the time). The lab thus switched to an interferometric approach, which was potentially cheaper, faster and more sensitive.
At around this time, Huang joined Fujimoto’s lab as a graduate student and was put on the LCI project. Fujimoto also invited Swanson, an MIT Lincoln Laboratory staffer working on intersatellite and fiber optic communications, to become part of the undertaking.
The contributions of both men proved central in different ways to the development of OCT. Huang had the key insight that hundreds of 1D optical echograms, or A-scans, coming out of the interferometric setup could be combined to build up a vertical cross-sectional image of the tissue at depth—a so-called B-scan or tomogram. Swanson, meanwhile, put his knowledge of optical-communications technology to work to create a compact, fast working prototype of a practical system. Swanson recalled to OPN, in a feature commemorating the technology’s 25th anniversary, that it was “a little surprising—the heart of an OCT system ended up looking very much like the intersatellite transceivers we were building” at the Lincoln Lab.
Expanding domains
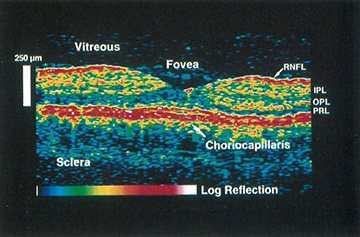
An early cross-sectional OCT retinal image from a human volunteer, reported in the 1993 paper in Optics Letters. [Image: E. Swanson et al., Opt. Lett. 21, 1864 (1993)]
The team reported its initial results in landmark papers in Science (1991) and Optics Letters (1993). Formal clinical trials, spearheaded by another researcher on the project, Carmen Puliafito, followed. Fujimoto, Swanson and Puliafito also established a company, Advanced Ophthalmic Diagnostics, to commercialize OCT, which was sold to the Carl Zeiss Company in 1994.
In the years since, the technology of OCT has experienced enormous success, spawning a billion-dollar-a-year market and affecting many millions of patients, particularly by revolutionizing retinal imaging and enabling the early diagnosis and treatment of retinal conditions.
Next-generation improvements such as time-domain OCT, spectral-domain OCT and swept-source OCT have refined the technique and expanded its usefulness in ophthalmology. And, growing out of those ophthalmological roots, OCT’s imaging domain has expanded to applications in cardiology, dermatology and gastroenterology—as well as some nonmedical areas such as industrial sensing and even art history and restoration work.
Interdisciplinary triumph
The Lasker Foundation, in its announcement of the award, notes that Fujimoto, Huang and Swanson’s achievement was the result of “stitching together optics, telecommunications engineering, and medicine.” Swanson, interviewed by OPN in 2016, likewise highlighted the interdisciplinary aspect of the achievement.
A lot of innovation “happens at the boundaries of disciplines,” Swanson told OPN. “OCT is such a rich combination of disciplines—in optics, mechanical systems, electronics, software, medical devices, clinical medicine. That’s one of the reasons there’s been so much innovation in OCT, and that there’s so much more to come.”
Correction: On 23 September 2023, at 10:45 EDT, the story was updated to include the color print version of the OCT image from the 1993 Optics Letters study by Swanson et al.

