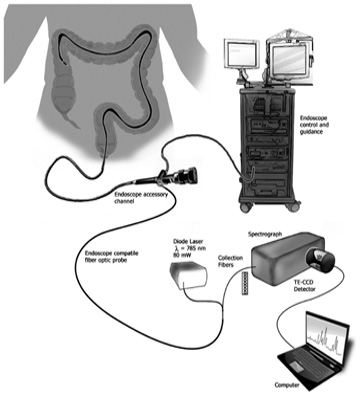
New Raman spectroscopy sensor detects molecular markers of IBD using a minimally invasive endoscope that can be easily integrated into a routine colonoscopy exam. [Image: Vanderbilt University] [Enlarge image]
U.S. researchers, led by Vanderbilt University’s Anita Mahadevan-Jansen, hope to improve the detection and classification of inflammatory bowel disease (IBD) with their new compact Raman spectroscopy probe—which is coupled to an endoscope that’s commonly used during colonoscopy exams (Biomed. Opt. Express, doi: 10.1364/BOE.8.000524).
In a recent pilot study, Mahadevan-Jansen’s team aimed to characterize the Raman spectral signatures of molecular markers for IBD and its subtypes, Crohn’s disease (CD) and ulcerative colitis (UC), and use these signatures to diagnose and differentiate IBD in human subjects.
Mahadevan-Jansen’s team says the results represent “significant progress toward improved real-time classification for accurate and automated in vivo detection and discrimination of IBD during colonoscopy procedures.”
Raman scattering for detecting inflammation
Raman scattering can capture the vibrational-mode “signature” of the chemical bonds in human tissue. In fact, Raman spectroscopy is already used to detect cancer in the gastrointestinal tract. According to the researchers, the technology can also be used to spot and distinguish changes associated with IBD and its subtypes’ inflammatory-response pathways.
To demonstrate this idea, the team designed and manufactured a Raman spectroscopy sensor small enough to fit into a colonoscopy endoscope. The sensor contained a 785-nm diode laser and a fiber optic probe that delivered 80 mW to the lining of the colon. To maximize collection efficiency at the probe tip, a plano-convex sapphire lens and MgF2 optical window sit in front of the probe’s filters. A lens filter was also added, to remove the scattering signal from the probe itself.
Before testing the device on human volunteers (UC, n = 8; CD, n = 15, control, n = 8), the team used tissue samples and animal models to characterize the spectral signatures for molecular markers associated with IBD and its subtypes.
Pilot study and results
During the volunteers’ colonoscopy procedures, the Raman spectroscopy probe was introduced through the endoscope accessory channel. Once in place, the probe applied 80 mW to the lining of the colon. The Raman scattered light was collected in reflectance mode and coupled to a spectrograph with a fixed volume-phase holographic grating, which provided spectral coverage from 450 to 1950 cm-1 and a resolution of 7 cm-1.
The researchers compared each volunteer’s spectra with the spectral signatures, and a physician’s evaluation based on standard endoscopy results, histopathology and patient history.
Overall, the study’s Raman spectra showed high sensitivity for identifying IBD (86 percent), but exhibited poor specificity for differentiating IBD subtypes (39 percent). However, the researchers devised a prediction algorithm that reached 90 percent sensitivity and 75 percent specificity for subjects with CD measured in the right colon segment.
The scientists are now refining algorithms to improve the test’s specificity, by incorporating data from a larger cohort of people to see how diet, gender, demographics and treatment type can affect the molecular markers associated with IBD.